At Clemson Eye, Dr. Peddada cares for patients with all types of diseases of the retina and is a specialist in the diagnosis and treatment of diabetic eye diseases such as diabetic retinopathy, diabetic macular edema, age-related macular degeneration (AMD), retinal vascular disease such as retinal vein occlusions resulting from systemic circulation problems, retinal tears/holes, other macular and vitreoretinal diseases.
Diabetic Retinopathy, an umbrella term for a number of conditions caused by high blood sugar, is the leading cause of new blindness in patients from 20 to 64.
Eye disease is a relatively lesser-known complication of diabetes, which contributes to a number of other serious eye conditions. For most diabetics, however, visual health can be preserved with a minor amount of effort. A regular annual eye exam can identify common eye diseases early before vision loss has occurred.
Diabetes affects nearly 14 million Americans and the number is growing. Diabetes affects 11 percent of South Carolinians and is the sixth leading cause of death.
Despite the prevalence of diabetes, 40 percent of diagnosed patients do not get an annual eye exam. Among seniors, nearly 44 percent believe failing vision is a normal part of aging and do not get a regular exam each year.
Diabetic eye disease and associated vision loss is preventable when detected early.
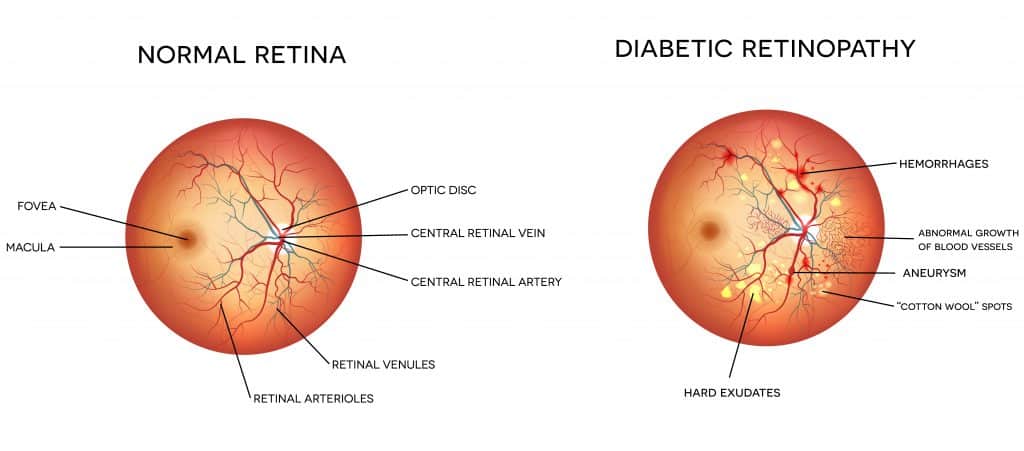
Diabetic Retinopathy is a group of related and serious conditions caused by high glucose levels that damage blood vessels in the eye. Diabetic retinopathy can progress through multiple stages. In the mild-to-moderate stages, swelling (called micro-aneurysms) occurs in the retina’s tiny blood vessels. This can leak fluid into the retina. As the disease progresses, tiny blood vessels can close off and lose their ability to transport blood to the retina. In the severe stage, called non-proliferative, more blockages occur, depriving the retina of its blood supply. And in the advanced “proliferative” stage, new, weaker blood vessels can form, eventually leading to bleeding, scarring, retinal detachment and permanent vision loss. A further complication is diabetic macular edema (DME). This is a buildup of fluid in the region of the retina that is responsible for clear, forward vision. The macula is critical for reading, recognizing faces and driving. According to the National Institutes of Health, about half of all diabetics with diabetic retinopathy will develop DME, the most common cause of vision loss among diabetic patients. Diabetes is also a contributing factor in other eye diseases such as glaucoma and the development of cataracts.
The prevalence of all types of retinopathy in the diabetic population increases with the duration of diabetes and the patient’s age. Most patients with diabetes ultimately develop abnormalities of the retinal blood vessels. Immediately after diagnosis of insulin dependent diabetes, no retinopathy is present. After seven years, 50% of patients have some degree of retinopathy. After 17‑25 years with the disease, 90% of patients have retinopathy. The prevalence of proliferative retinopathy is 26% after 26‑50 years duration of diabetes. In addition, systemic hormonal changes at puberty result in the increased prevalence of retinopathy after age 13.
New drug development and the technology to deliver them effectively have revolutionized the care of patients with diabetic eye diseases. Many patients with diabetic retinopathy see vision improvements or stability after intravitreal injections of a new range of drugs known as anti-VEGF (vascular entothelial growth factor). These drugs stop or slow the production of proteins that contribute to the growth of blood vessels. Reducing new blood vessel growth also slows down the attendant leakage and swelling these vessels can cause. That can slow down vision loss and stabilize your visual health.
Medication is injected into the vitreous, the jelly-like fluid that fills the inside of the eye. The procedure may need to be performed more than once and your Clemson Eye ophthalmologist will go over the optimum schedule with you. Most health plans cover these injections as a medical expense. Patients with diabetes are 40 percent more likely to have Glaucoma, caused by pressure building up in the eye.
An exciting new technology called the iStent has only recently been approved by the FDA. And Clemson Eye is one of a handful of ophthalmologists certified to perform this procedure in South Carolina. At 1 millimeter long, the iStent is the smallest device approved for implantation in the body. Like other stents, it bypasses blockages and relieves pressure in the eye. This can reduce or even eliminate the need for drops, according to Dr. Joseph Parisi, chief ophthalmologist and medical director. So far, 68 percent of patients have stayed medication-free, a significant benefit since drops can be both painful and expensive. It has also been shown in clinical studies that specifically formulated Omega-3 fatty acids can help reduce the risk and slow the advancement of diabetic retinopathy.
As many as 74% of people with diabetes could have difficulty digesting dietary fats including Omega-3s. Nuretin® is a specifically formulated medical food that provides the right balance and dose of Omega-3 fatty acids in highly absorbable form to ensure that you are able to utilize Omega-3 essential fatty acids for protecting your eyesight.
Table 1 shows the quantity, pricing, and dosage of the Omega-3 containing Nuretin.
| Quantity | Recommended Dosage | Price (Per Bottle) * |
|---|---|---|
| 56 | 2 per day | $34.95/bottle |
The Panretinal Laser Photocoagulation procedure is used for the treatment of the peripheral retina to help reduce the potential for vision loss as a result of PDR.
Treatments are most effective if they can be initiated preventively – before vision is lost. People with diabetes should have their eyes examined at least once a year to make sure they do not have early damage. If you have diabetes and experience any change in your vision, do not chalk it up to normal aging. Book an immediate appointment with your Clemson Eye doctor. If you are pregnant when diagnosed with diabetes, you should have an eye exam immediately. The Centers for Disease Control estimates that 28 percent of the population have undiagnosed diabetes. So you may not know that you have the disease, making an eye exam even more important. Every year.
Although diabetes cannot be prevented, in many cases its blinding complications can be moderated. Unfortunately, many diabetic patients’ eye health is not managed appropriately. Many high-risk diabetes patients do not receive vision-saving treatment. One study showed that 11% of Type I and 7% of Type II patients with high-risk retinopathy have not even been seen by an eye doctor in the past two years. Table 1 shows the recommended schedule for initial and follow‑up examinations based on time of onset of diabetes.
Macular Degeneration occurs when there is damage to the macula inside your eye causing you to lose central vision making depth perception difficult.