Keratoconus is a bilateral (both eyes) degenerative condition of the cornea, the transparent dome-shaped tissue that forms the front part of the eye. Keratoconus is a condition in which the cornea progressively becomes thinner, weaker, and irregular in shape.
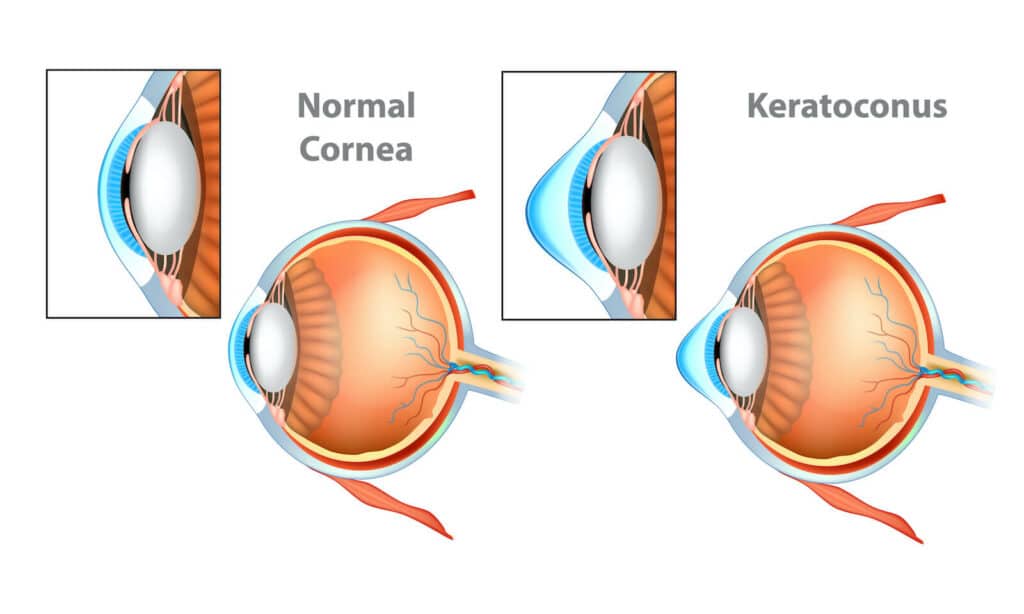
Instead of a normal, relatively round shape resulting in clear vision, the cornea in keratoconus can become cone-shaped. This can interfere with the ability to see clearly, resulting in a distorted image being projected onto the brain. Because the cornea is irregular and cone-shaped, glasses do not adequately correct the vision in patients with keratoconus since they cannot conform to the shape of the eye.
Patients with keratoconus see best with rigid contact lenses since these lenses provide a clear surface in front of the cornea, allowing the light rays to be projected clearly to the retina. This is how most cases of keratoconus are treated. However, there are some excellent new surgical options for patients with keratoconus who cannot tolerate these lenses.
Many patients are initially unaware they have keratoconus and see their eye doctor because of increasing blur or progressive changes in their prescription. Keratoconus may occur in one eye only initially, but most commonly affects both eyes, with one eye being more severely affected than the other. Both males and females, and all ethnicities are equally affected.
The treatment approach to keratoconus generally follows an orderly progression from glasses to contact lenses to corneal transplantation. Glasses are an effective means of correction for mild keratoconus. As the cornea steepens and becomes more irregular, glasses are no longer capable of providing adequate visual improvement. Corneal transplant surgery is indicated when a patient cannot wear contact lenses for an acceptable period of time or when the vision, even with contacts, is unsatisfactory.
A gas permeable contact lens is the most highly effective way to manage keratoconus, and 90% of all cases can be managed this way indefinitely. The use of gas permeable contact lenses has been the mainstay of the optical management of keratoconus. These lenses, manufactured in a large variety of unique designs, provide a regular surface over the cornea to neutralize the distortion brought on by the irregular cornea.
No one design is best for every type of keratoconus. Since each lens design has its own unique characteristics, the practitioner needs to carefully evaluate the needs of the individual and find the lens that offers the best combination of visual acuity, comfort, and corneal health. Fitting contact lenses for keratoconic eyes is by no means simple. Numerous lenses are often fit, and it can take a great deal of time. If the cornea becomes too scarred or painful, a corneal transplant may be necessary.
Corneal Collagen Crosslinking, also known as CXL, is an in-office keratoconus treatment procedure that strengthens the collagen fiber bonds within the cornea to halt the progression of the dome-like bulging. With keratoconus, the cornea is structurally weak, and collagen fibers within the cornea have too few crosslinks.
The crosslinking process involves applying Vitamin B2 (riboflavin) eye drops to the cornea. Once the riboflavin has been absorbed by the cornea, a highly precise, low dose of ultraviolet light is directed at the cornea for 20 to 30 minutes. This procedure takes place in a single treatment.
Corneal collagen crosslinking is a chemical process similar to the vulcanization of soft rubber to strengthen it into the strong rubber that makes up a tire. Unlike vulcanization, corneal crosslinking uses a weak beam of ultraviolet light and Vitamin B2, and the strengthening process happens at normal body temperature. Within minutes, the strengthening process has occurred.
Crosslinking has been practiced worldwide since 1998, although Clemson Eye was the first in South Carolina to bring this technology to their patients. If you have keratoconus, you’ve got access to a leading expert… right here in the Upstate!