Posted by: Clemson Eye in News

By Brian Johnson, MD
Clemson Eye News, October 2016
Dry Eye affects an estimated 25 million Americans and is the most common reason for a visit to an eye specialist. It is a complex disease involving the tear quantity, quality, inflammation, and eyelid oil or Meibomian Gland Dysfunction (MGD).There are several dry eye symptoms such as a stinging, burning or scratchy sensation in your eyes, stringy mucus in or around your eyes, sensitivity to light, eye redness, difficulty wearing contact lenses, difficulty with nighttime driving, and watery eyes, which is the body’s response to the irritation of dry eyes.
Causes
Over the past 15 years, research has revealed that Meibomian Gland Dysfunction is the leading cause of eye discomfort for over 86% of patients with Dry Eye. The Meibomian Glands of the upper and lower lids play one of the biggest roles in dry eye symptom management. The Meibomian glands produce specific lipids (a clear oil) that coat and cover the tears which prevents them from evaporating. The meibomian glands can get obstructed with bacteria, cholesterol, debris, allergens and even make-up. Additionally, incomplete blinking caused by staring at devices such as computers and smart phones can lead to the glands being obstructed.
Other causes include age, medications, health
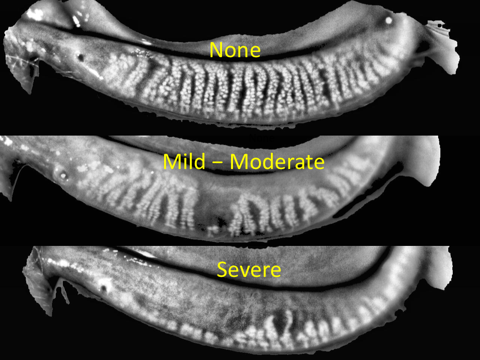
Photo of Meibomian Glands
“Unaddressed, dry eyes can become symptomatic and cause significant discomfort as well as decreased or fluctuation vision. Permanent changes can occur to the cornea and structures of the eyelid, leading to irreversible damage.” says Dr. Brian Johnson, Ophthalmologist at Clemson Eye.
Testing
Several tests are used to determine if MGD is causing Dry Eye. Meibography enables critical analysis of the structural integrity of the lipid producing glands of the lid. The Meibomian Gland Evaluator measures the function of the glands during normal blinking. This test also examines the quality of the meibomian secretions and helps to establish a course of treatment. The Light Test diagnoses whether the lids are properly sealing to prevent exposure desiccation.
MGD is a progressive disease that leaves in its wake permanent structural damage. This is because once the Meibomian Glands become clogged they begin to deteriorate. First the glands dilate, and then shorten, finally they atrophy. Therefore, our doctors routinely test for MGD.
Treatment
Traditional treatment includes artificial tear drops and lifestyle changes, but there are some advanced therapies. During a dry eye exam, the doctor will check to see if the glands are releasing oil during the blinking process. The Lipiview® test provides an accurate digital image of the Meibomian glands and blink function. If the test shows the gland function has dropped off and there is ‘Evaporative Dry Eye’, then the doctor will recommend cutting edge treatment either with a LipiFlow® or other therapies such as prescription anti-inflammatories, Restasis, Xiidra, omega-3 supplements, Prokera, or punctal plugs.
LipiFlow® is the only electronic device cleared by the FDA for treatment of MGD with clinical studies of safety and effectiveness. Through advances in the application of Vectored Thermal Pulsation (VTPTM) technology, LipiFlow® utilizes a patented algorithm of precise heat applied to the inner eyelids with directed gentle massage to remove blockages from the Meibomian glands. This treatment is designed to restore the natural oil flow to the tear film that covers the eye’s surface and save the glands.
Overall, Dry Eye treatments may make a sufferer more comfortable and often improve the quality of vision. Anyone with symptoms of Dry Eye should visit an eye care professional specializing in Dry Eye treatment.
Dr. Brian Johnson is an Ophthalmologist at Clemson Eye.
What’s New
LASIK uses lasers to correct vision problems like nearsightedness, farsightedness, and astigmatism. It is the most popular refractive surgery performed in the United States and considered the safest elective procedure in all of medicine. Laser vision correction gives you great vision, generally restoring 20/20 vision and eliminating or reducing reliance on glasses and contacts.
Clemson Eye is a well‑respected leader in laser vision correction, having treated more than 15,000 Upstate patients to freedom from glasses and contacts. Not all LASIK procedures are created equal. Some outcomes are better than others, depending on many factors, including the equipment and technique used. In 2016, Clemson Eye purchased a topography guided laser system called Contoura Topography-Guided LASIK. It is the most advanced laser vision correction in the nation.
Recently FDA approved, Contoura is a step into the future. The system uses advanced technology to incorporate a patient’s prescription and corneal irregularities into a highly customized map of their eye. It plots approximately 22,000 points of curvature on the cornea (front part of eye) versus 168 points through traditional topographers, allowing for greater customization and accuracy in treating the prescription or refractive error. While these advancements improve surgical planning and visual outcomes for all LASIK patients, they are particularly beneficial to patients with irregular corneas caused by past surgery, eye disease or corneal scarring due to contact lens wear. Results from a recent study¹ exceeded expectations. When treated with a topography guided system, 92.7% of all patients achieved an uncorrected visual acuity (UCVA), that is vision without glasses, of 20/20 or better, and 68.8% achieved a UCVA of 20/16 three months after surgery. ²
Symptoms traditionally associated with LASIK, such as glare, halos, difficulty driving at night, light sensitivity and eye dryness, also improved after

Topoguided Lasik Scan
1. Results from FDA T-CAT-001 clinical study for topography-guided vision correction (with the 400 Hz ALLEGRETTO WAVE® Eye-Q Excimer Laser).
2. Post hoc analysis of postoperative UCVA compared to preoperative BSCVA of 230 eyes contained in the FDA T-CAT pivotal trial at 12 months. The primary end point evaluated changes in BSCVA.
Click here to view and download this article [PDF]